Neck of Femur Stress Fracture
- Best Asics Shoes for Flat Feet - October 25, 2024
- Best Running Shoes for Flat Feet - October 22, 2024
- Posterior Tibial Tendonitis - October 21, 2024
Overview
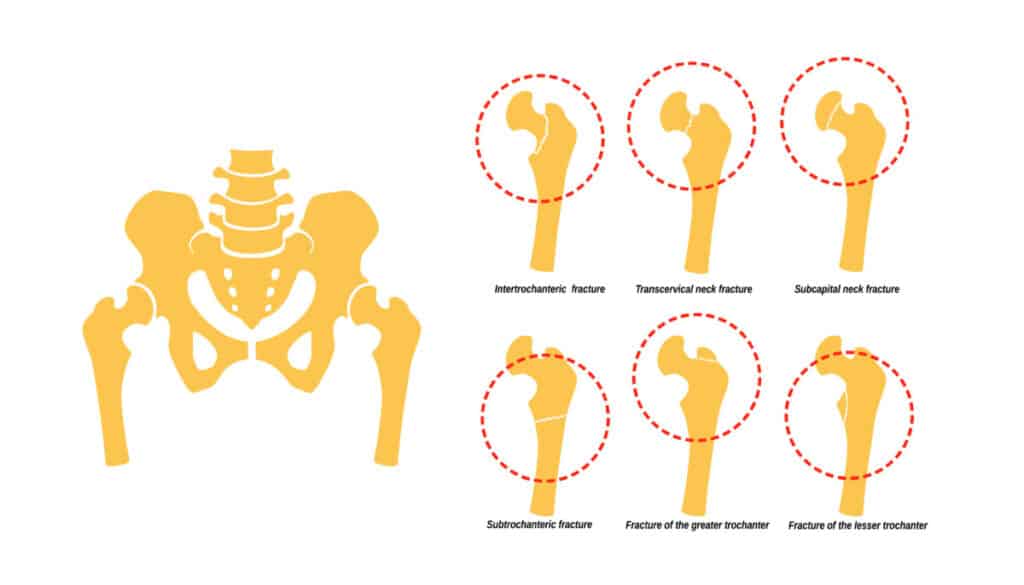
Neck of Femur Stress Fracture is a relatively uncommon condition that predominantly affects marathon and long-distance runners. The femoral neck is the portion of the femur that sits between the femoral head (which articulates with the acetabulum to form the hip joint) and the femoral diaphysis (i.e. the thigh bone).
Causes
Bones are subjected to constant processes of degradation and remodelling throughout their life span. Bones need to meet mechanical needs during certain sports or daily activities.
In a healthy state, the remodelling process outweighs the degradative process, thus accumulating healthy bone tissue. Conversely, when an excessive loading is placed on a bone, degradation may take over and weaken the bone over time.
The risk for this is the development of a bone stress reaction, with some inflammation and little effect on bone structure. The other end of the spectrum is an actual fracture in the area where the bone has become weaker.
Risk Factors
Several risk factors have been implicated in the development of a stress fracture. We have mentioned previously that an unaccustomed amount of loading, particularly running volume, may be the primary driver for developing a stress fracture.
Nonetheless, other systemic factors should be considered to increase suspicion of a stress fracture. Women seem to be more predisposed to the development of a hip stress fracture than men.
Problems with the menstrual cycle (amenorrhea, dysmenorrhea) create hormonal imbalances that could negatively affect bone health. Likewise, a poor diet with low levels of vitamin D and calcium intake may also affect the ability of bones to cope with loading.
Symptoms
Symptoms of a femoral neck stress fracture involve gradual worsening of hip or groin pain, generally perceived at the front of the hip. It usually starts with pain at the end of a run, with a gradual worsening that impacts sports participation. Rest seems to be the only easing factor.
Ultimately, there may be pain upon any impact activity and throbbing pain at night that may wake you up. There may be radiating pain to the knee and the glutei area.
Diagnosis
Diagnosis of femoral neck stress fracture involves a thorough history of training load, particularly changes in training volume and intensity. In addition, assessing those systemic factors outlined earlier is essential to increase the index of suspicion.
Physical examination involves testing hip mobility, with potential discomfort at the end ranges of hip internal rotation and hip flexion. Pain on hopping is probably the best clinical test available to reliably rule in or out a femoral neck stress fracture.
If there is no pain on hopping, it is pretty unlikely you currently have a femoral neck stress fracture. Clinical symptoms should also be correlated with an MRI investigation for a complete diagnosis.
Treatment
If a femoral neck stress fracture is suspected, we must understand the type of fracture we are dealing with. A compression-type stress fracture at the bottom of the femoral neck should be treated conservatively with 6 weeks of complete off-loading on crutches.
During this time, non-weight-bearing exercises should be prioritised to avoid de-conditioning the whole lower limb. Cross-training, including pool work and upper limb aerobic conditioning, should complement rehabilitation.
After this period, a gradual return to partial and full weight-bearing should commence, guided by pain.
On the other hand, fractures of the upper portion of the femoral neck are more severe and may require surgical stabilisation. If left untreated, a fracture in this area may compromise the vascular supply of the femoral head and lead to avascular necrosis, which requires hip replacement surgery.
__________________________________
We specialise in treating shoulder conditions such as femoral fractures and have lower limb experts who can help you in our Fulham, southwest London clinic.
Related Articles
Hip Pain Running – How long after THR before I can ski? – Hip Flexor Tendonitis
We offer Online Appointments for £60 and Face-to-Face appointments for £85 in our clinics.
