Proximal Hamstring Tendinopathy
- Proximal Hamstring Tendinopathy - January 20, 2022
What is a proximal hamstring tendinopathy?
Proximal Hamstring Tendinopathy is a common condition that mid to long-distance runners and sprinters encounter. Symptoms usually present during sports, with a gradual onset of pain around your sitting bones.
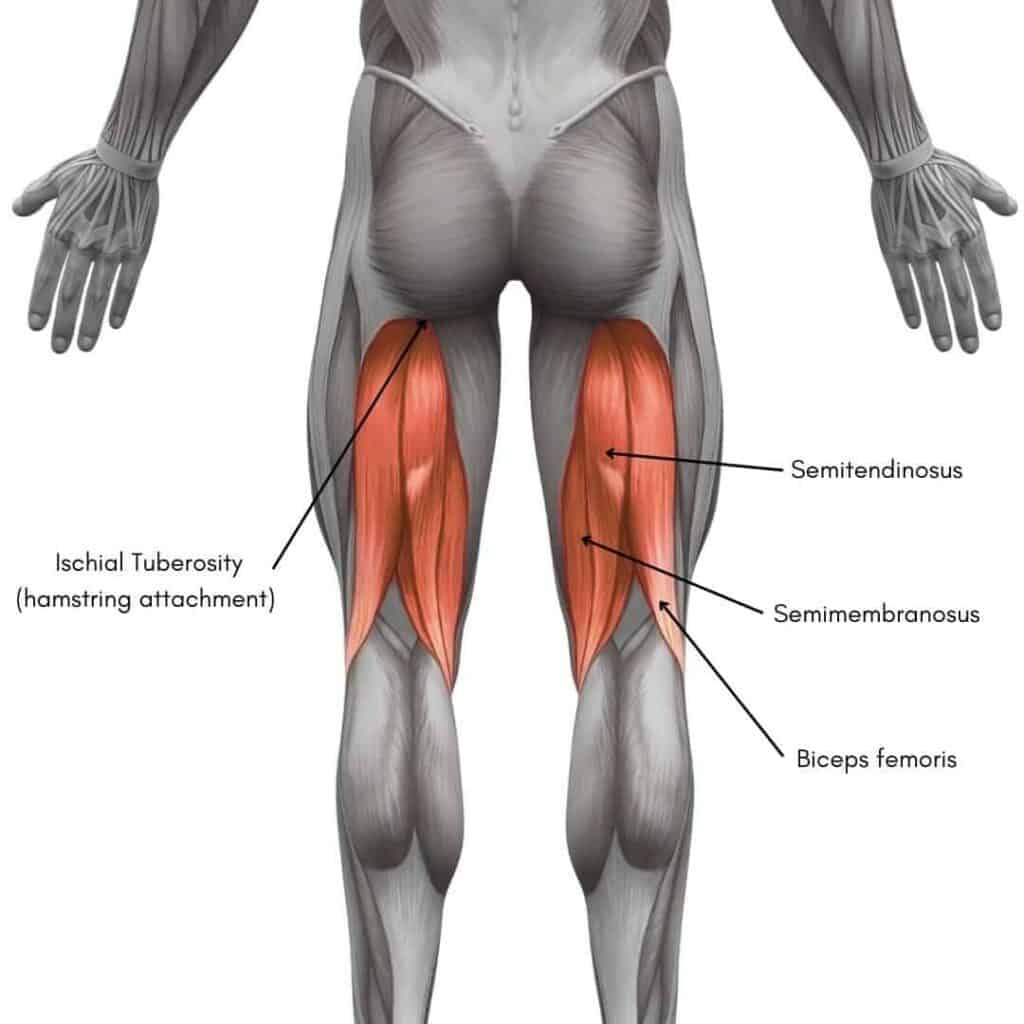
The anatomical name for the “sitting bone” is the ischial tuberosity, which is an important bony protuberance that provides attachment to three different hamstring muscle tendons. Between these and the ischial tuberosity lies the ischiogluteal bursa, which can also be partially responsible for the symptoms.
What are the possible causes?
A sudden increase in running volume, intensity, and speed training are the primary causes of Proximal Hamstring Tendinopathy. Notably, the sudden introduction of hill work due to increased hip flexion may sensitise the proximal hamstring tendons or the bursa.
An easy way to prevent this is to allow enough time for tendons to adapt to new training stimuli. Cross-training and consistent planning of recovery weeks are considered best practices.
Symptoms
The most common symptom is pain on the seat bone, sometimes described as just on the inside of the seat bone. This may also feel like stiffness, tightness or fatigue in this area.
The whole hamstring may feel tight, but usually, the seat bone will be the point where the most tightness is felt when stretching.
Symptoms are aggravated by compressive or sheering forces at the ischial tuberosity. This includes sitting, especially if on a hard surface, high angles of hip flexion, sprinting, running up hills and stretching the hamstring.
Treatment options
In most cases, treatment with a specific rehabilitation exercise programme will effectively and successfully reduce pain and strengthen the proximal hamstring tendon. So long as aggravating activities are modified, reduced or stopped.
Nonsteroidal anti-inflammatory medication can also play a role in symptom relief. Still, it should not be used in the very early, acute phase as they can stop inflammation’s positive effects on healing (Su & O’Connor, 2013).
If rehabilitation exercises are not practical or there is time pressure on recovery, then additional treatment can be used, such as extracorporeal shockwave therapy. In a very small number of cases, steroid injections can be used. Caution must be taken with steroid injections as they can harm tendon tissue health.
All of these additional treatments will not be effective on their own. All treatments must be used along with a comprehensive and specific strengthening programme for the hamstrings and surrounding muscles.
Proximal Hamstring Tendinopathy Exercises
At the initial stages, long-held hamstrings and glutes isometric contractions should be preferred, in order to provide an analgesic effect whilst loading the tendons. Contractions should be held for around 30-40 seconds, whilst the intensity of the exercise should be increased as pain allows. Minimal pain should not be feared during the exercises, provided it settles quickly after the session. Examples of these are:
- Isometric double-leg bridge
- Isometric double-leg bridge with elevated feet
- Isometric double-leg bridge on a Swiss ball
- Isometric single-leg bridge
Consequently, heavier exercises involving hip flexion should be commenced. These can include:
- Good morning exercise with weights
- Double-leg Romanian Deadlift
- Arabesque
- Single leg squats
- Prone Hamstring Curl Machine

Lastly, plyometrics and power activities should be performed. These may involve hopping, landing, high knee drive and heel flicks.
Exercises to Avoid with Proximal Hamstring Tendinopathy
During the acute phases of Proximal Hamstring Tendinopathy, it is best to avoid the following exercises to reduce the risk of exacerbating your symptoms:
- High Step Ups
- Deep Squats
- Running Uphill
- Hamstring Stretches
- Straight Leg Deadlifts
Can I run with proximal hamstring tendinopathy?
In our experience, yes, you can continue to run, but it can depend on the circumstances. In irritable cases, with symptoms at rest or during simple walking, it is best to cease running for a couple of weeks to allow symptoms to settle.
In less irritable presentations, with pain that comes along 30 minutes into your run, running for 20 minutes at a slow speed and on a flat surface is okay. Hills may aggravate your pain by further sensitising the bursa and the tendons.
We offer Online Appointments for £60 and Face-to-Face appointments for £85 in our clinics.
Related Articles:
Hip Bursitis Overview – Hip Bursitis Exercises to Avoid – Hip Labral Tear
