Total Hip Replacement (THR)
- Best Asics Shoes for Flat Feet - October 25, 2024
- Best Running Shoes for Flat Feet - October 22, 2024
- Posterior Tibial Tendonitis - October 21, 2024
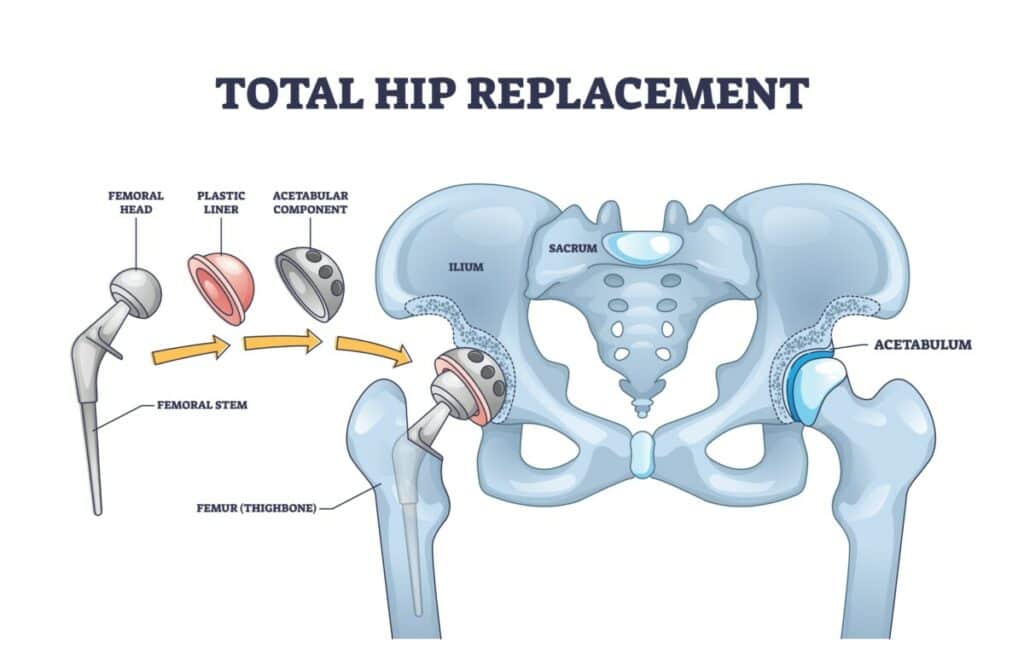
A total hip replacement is an orthopaedic procedure that involves replacing the head of the femur and the acetabulum of the pelvis with artificial components.
These components replicate the ball and socket of the hip joint and are commonly crafted from metal, ceramic, or plastic. A less invasive alternative to total hip replacement is hip resurfacing, in which only a minimal amount of bone is removed from the femur and pelvis.
The Birmingham hip resurfacing method is the most prevalent of these techniques. Instead of replacing the entire joint, this method only replaces the surfaces of the femoral head and the acetabulum. Younger patients often favour it, as it conserves more of the natural bone, paving the way for potential future surgeries—essential considering the finite lifespan of prosthetics.
Reasons Why You Might Have a Total Hip Replacement?
Trauma
A fracture in the femur or acetabulum can often be addressed using pins and plates to stabilize the bones, aiding in their healing. However, in situations where there’s reduced bone density, such as with osteoporosis or osteopenia, the healing process may be compromised. In such cases, a total hip replacement might be the advisable course of action.
Osteoarthritis
The primary reason for elective total hip replacement surgery is joint degeneration, which results in pain and limited mobility. When this significantly impacts one’s quality of life and activity levels, and if physical therapy fails to offer notable improvements, a total hip replacement surgery becomes a viable option.
Congenital Hip Dysplasia/Perthes Disease
Certain congenital conditions affect the formation of the hip joint in childhood and adolescence. Poor structure and shape can result in early degeneration of the hip and early onset osteoarthritis. Therefore, these individuals are likely candidates for a total hip replacement.
Surgery
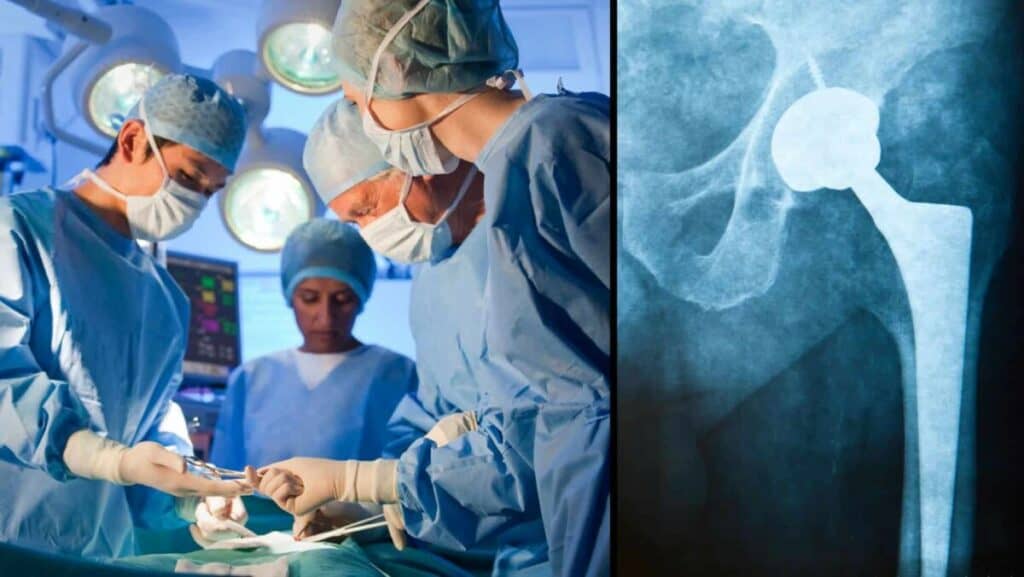
Opting for a total hip replacement is a significant medical decision, and one should give it profound consideration, evaluating the potential risks and benefits. This procedure, which involves replacing a damaged hip joint with an artificial one, has seen significant advancements.
The recovery trajectory has dramatically improved with the evolution of surgical techniques, state-of-the-art prosthetics, and more sophisticated post-operative physical therapy regimens. As a result, patients, especially those who maintain good health, physical fitness, and muscular strength, can anticipate a better recovery process.
From a medical standpoint, elective surgeries, those scheduled in advance rather than in an emergency, are typically more advantageous. Planning allows the patient ample time for thorough pre-operative assessments, optimising their physical condition, and undergoing necessary medical interventions to ensure the best surgical outcome.
Pre-Operative Physical therapy
Often referred to as prehab, this is the physical training undertaken before surgery. Pre-operative Physical Therapy can include strengthening exercises for muscles around the hip, which will help recovery, and learning the exercises and movements that might have been unfamiliar and will be part of your post-operative rehabilitation.
Post-operative physio follows strict protocols to ensure the surgery has the best opportunity to be successful. There are common limitations to the ranges of movement of the hip as well as activities that are evidence-based and should be followed closely.
There are also specific limitations and restrictions that a surgeon might impose to reflect the specifics of the surgery procedure and the individual’s anatomy and risks. Many people are surprised with how quickly they are expected to get out of bed and start walking.
The hip joint is very stable, and weight-bearing in a standing position is safe and the best way to start strengthening and returning to functional activities.